HEMANGIOSARCOMA
BACKGROUND
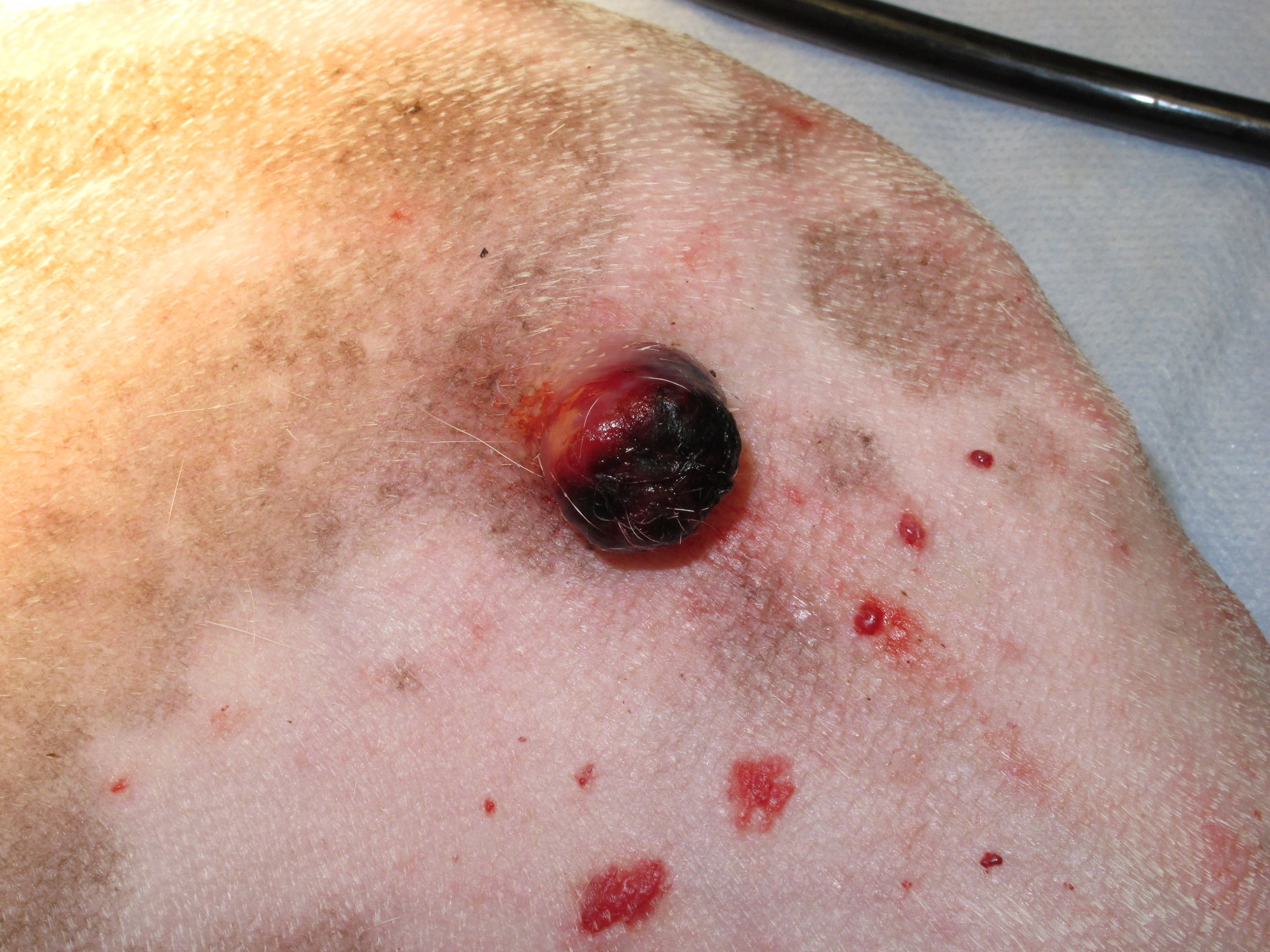
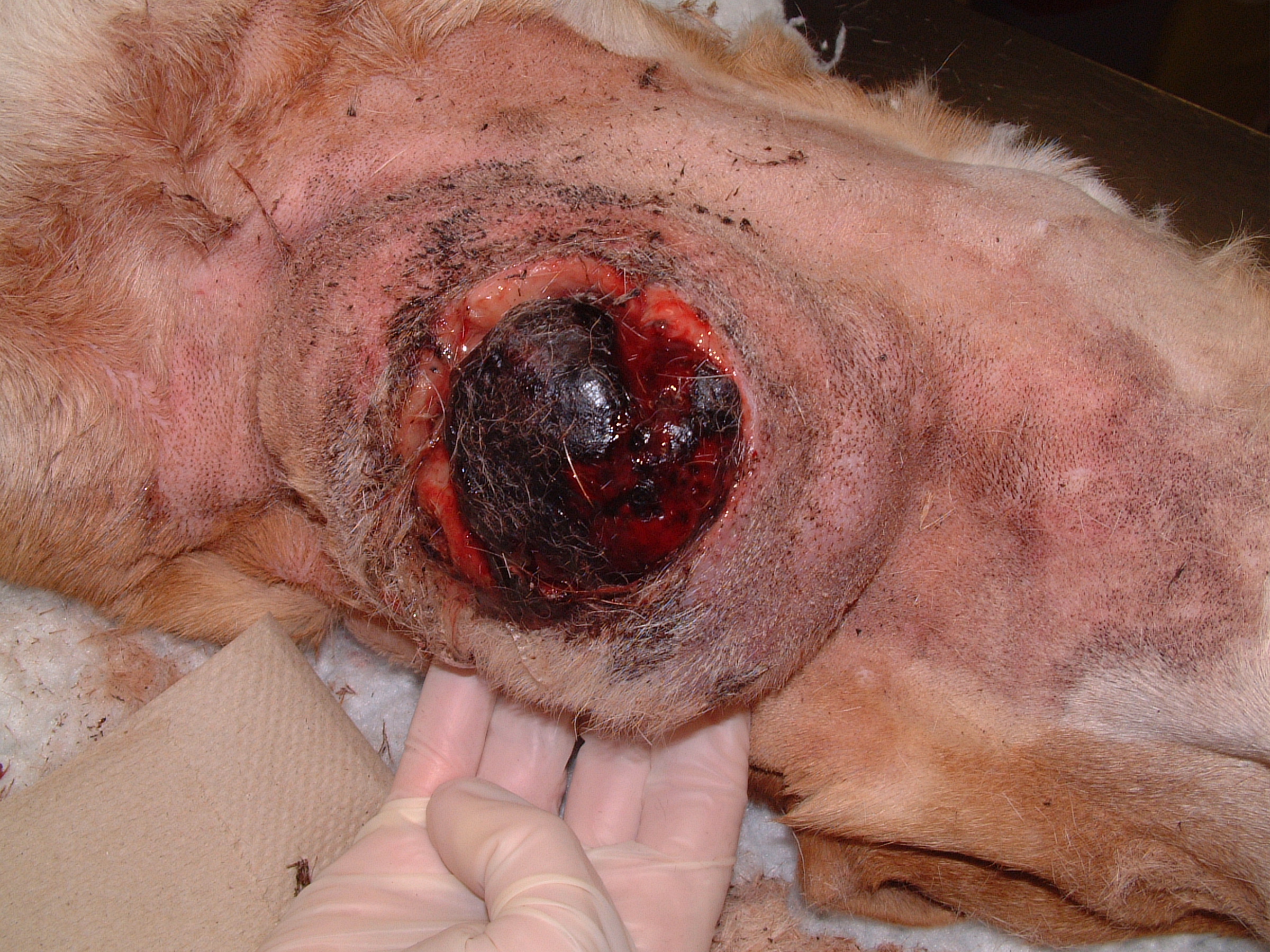
Hemangiosarcoma (HSA) is a common malignant tumor arising from vascular endothelial cells. The most common site of primary HSA in dogs is the spleen; however, HSA arises primarily from the skin, subcutaneous tissue, or muscle in 13%-47% of dogs. In one study of 212 dogs (1992), benign hemangiomas (73%) were more common than malignant HSA (27%); and HSA arose more commonly in the skin (73%) compared to subcutaneous tissue (7%). Cutaneous HSA frequently arises along the ventral abdomen and inguinal region in short-haired dogs and exposure to ultraviolet radiation is suspected as the cause of cutaneous HSA in these dogs. Cutaneous HSAs are often solitary, but multiple cutaneous HSA lesions are reported in 18%-29% of dogs. Clinically, cutaneous HSA are often poorly circumscribed and ulcerated.
Cutaneous and subcutaneous HSA are also relatively common in cats, but most dermal HSAs in cats are solitary.
DIAGNOSIS
Fine-needle aspirates or incisional biopsy are required for the preoperative diagnosis of HSA. Fine-needle aspirates can be non-diagnostic because of blood contamination.
CLINICAL STAGING
Ultrasound or CT scans of the tumor are occasionally recommended to determine the extent of the local tumor and assist in surgical planning, especially for intramuscular HSA. Metastasis to the lungs and intra-abdominal organs is relatively common for subcutaneous and intramuscular HSA, so three-view thoracic radiographs or thoracic CT scan are recommended for the assessment of pulmonary metastasis, and abdominal ultrasonography or CT scan are recommended for assessment of intra-abdominal metastases.
TREATMENT
Surgical excision is recommended for cats and dogs with cutaneous, subcutaneous, and intramuscular HSA. The margins required for complete histologic excision are unknown, but 3cm lateral margins and one fascial layer for deep margins are recommended because of the relatively high rate of local tumor recurrence following less aggressiuve surgical approaches. Postoperative chemotherapy is recommended for dogs with subcutaneous and intramuscular HSA.
PROGNOSIS
Dogs - Cutaneous HSA
The prognosis for dogs with HSA depends on the location of the HSA and treatment. In general, the prognosis is better for dogs with cutaneous HSA compared to either subcutaneous or intramuscular HSA. In one clinical paper (1994) of 25 dogs with dermal HSA treated with surgical excision alone, the median survival time for dogs with cutaneous HSA (780 days) was significantly better than dogs with either subcutaneous (172 days) or intramuscular HSA (307 days). In a clinical study of 94 dogs with cutaneous HSA treated surgically (2012), local tumor recurrence was reported in 77% of dogs with a median time to local recurrence of 211 days. Local tumor recurrence was significantly more common in predisposed breeds (Whippet, American Staffordhsire Terrier, Pitbull Terrier, Italian Greyhound, Beagle, and Dalmation), ventral tumor location (i.e., solar-induced cutaneous HSA), and dogs with multiple cutaneous HSAs. The completeness of histologic excision and invasion into subcutaneous tissue were not associated with an increased risk of local recurrence in this study. The distant metastatic rate for dogs with cutaneous HSA is 30%-34% with a median time to metastasis of 326 days. In an earlier study, the most common site of metastasis was other cutaneous sites, but a site distrubition of metastasis more consistent with visceral HSA (liver, spleen, lungs, heart, bone, and central nervous system) was reported in a later study. Distant metastasis was significantly less likely in predisposed breeds and significantly more likely in dogs with invasion into subcutaneous tissue. The overall median survival time for dogs with cutaneous HSA was 780-987 days with 1-, 2-, and 3-year survival rates of 79%, 60%, and 44%, respectively. Prognostic factors include predisposed breeds (median survival time 1570 days compared to a median survival time of 593 days in non-predisposed breeds), ventral abdominal location (median survival time 1085 days compared to a median survival time of 539 days for cutaneous HSA in other locations), and solar-induced cutaneous HSA (median survival time 1549 days compared to a median survival time of 545 days in dogs without solar-induced changes).
Dogs - Subcutaneous and Intramuscular HSA
The prognosis for dogs with subcutaneous and intramuscular HSA is significantly worse than cutaneous HSA. The prognosis is worse because HSA arising from these deeper locations have a higher metastatic rate (43%-73%). In one clinical study (2011) of 71 dogs with subcutaneous (n=65) and intramuscular (n=16) HSA, the overall median survival time was only 172 days with 1- and 2-year survival rates of 25% and 4%, respectively. There were different treatment groups, but most were treated with surgery alone. Dogs treated with surgery had a median survival time of 246 days and dogs with good local tumor control (defined as either surgery alone with complete histologic excision or surgery with incomplete histologic excision combined with radiation therapy) had a median survival time of 399 days. Other prognostic factors included tumor size (with median survival times of 364 days for tumors < 4 cm, 212 days for tumors 4 cm to 6 cm, and 130 days for tumors > 6 cm), metastasis at diagnosis (median survival time 115 days), and gross residual disease after treatment (median survival time 89 days). Survival outcomes are better when surgery is combined with chemotherapy, at least for dogs with subcutaneous HSA. In one study of 21 dogs with subcutaneous (n=17) or intramuscular HSA (n=4) treated with surgery and adjuvant doxorubicin chemotherapy (2008), the median survival times for dogs with HSA in subcutaneous and intramuscular locations were 1189 days and 273 days, respectively. Dogs with subcutaneous HSA had significantly longer median disease-free intervals and survival times compared to dogs with intramuscular HSA; and dogs with subcutaneous HSA and < 9 years old also had significantly longer median disease-free intervals and survival times compared to older dogs.
Cats
In one study of 18 cats with cutaneous and subcutaneous HSA (2005), surgery was performed in 10 cats with 1cm-3cm surgical margins. Despite this relatively aggressive approach, only 50% of these resections had complete histologic excision. All cats with complete histologic excision were alive and disease-free at the end of the study (range, 120-1186 days). Of the cats with incomplete histologic excision, only one cat developed local tumor recurrence (at 270 days) and none of the remaining cats developed either local tumor recurrence or distant metastasis (range, 90-1460 days). The overall median survival time in this study was 912 days and cats treated surgically had a significantly increased median survival time (not reached and > 1460 days because only one cat died of tumor-related reasons) compared to cats not treated surgically (60 days).
Cutaneous and subcutaneous sites were the most common sites for HSA in another study of 53 cats with HSA, with HSA arising from the skin in 24 cats, subcutaneous tissue in 17 cats, and visceral sites in 10 cats. The majority of cats were treated with surgery and complete histologic excision was achieved in 73% (17/23) of cats with cutaneous HSA and only 6% (1/16) of cats with subcutaneous HSA. Local tumor recurrence was reported in 50% of cats with incomplete histologic excision with a median time to local recurrence of 208 days. Metastasis was not reported in cats with cutaneous HSA, but was either diagnosed or suspected in 24% (4/17) cats with subcutaneous HSA. The overall median survival time was 283 days. Prognostic factors included tumor location, histologic margins, and mitotic rate. Cats with cutaneous HSA had significantly longer survival times (median survival time not reached with no cat dying of tumor-related reasons) than cats with subcutaneous HSA (median survival time 384 days) and visceral HSA (median survival time 0 days). Cats with complete histologic excision had significantly longer survival times (median survival time not reached with no cat dying of tumor-related reasons) than cats with incomplete histologic excision (median survival time 274 days). Finally, cats with a mitotic index of 3 or less had a median survival time that was not reached compared to a median survival time for 60 days for cats with a mitotic index greater than 3.
Last updated on 6th March 2017